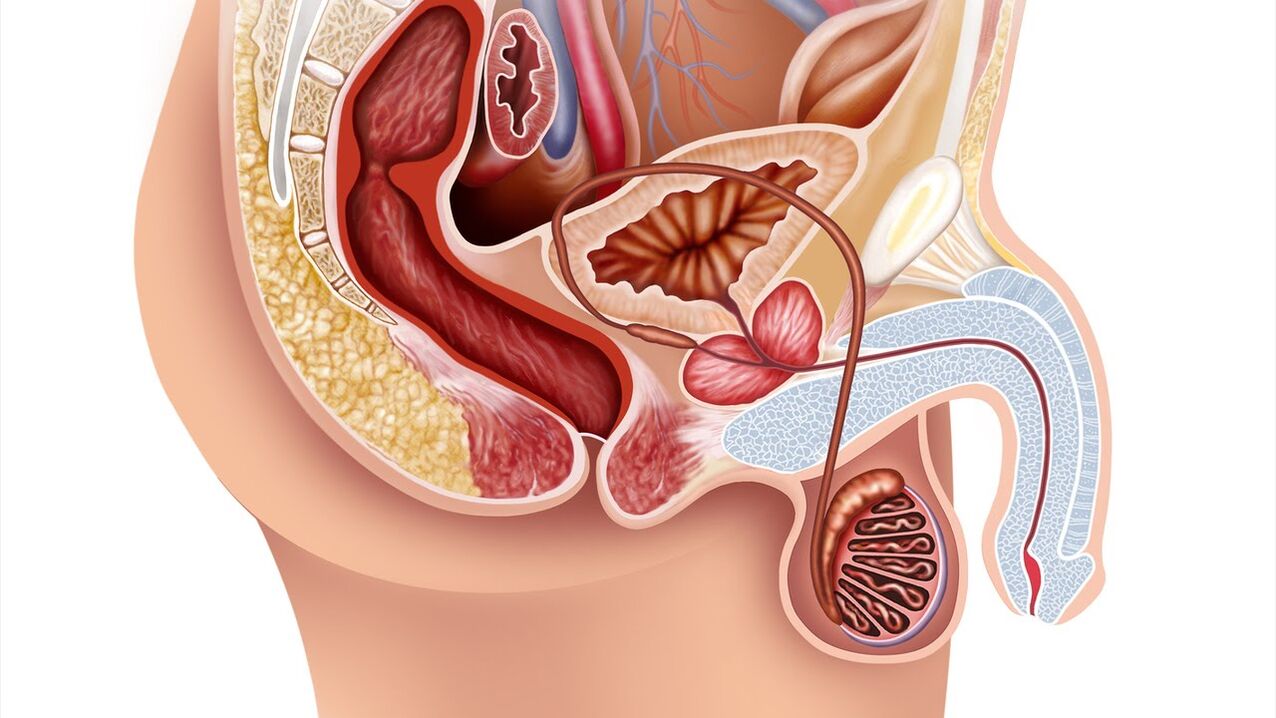
Prostatitis is an inflammatory process associated with inflammation of the prostate gland (prostate) in males. Most often this disease occurs in men over 30 years of age. This ailment causes pain in the lower back, perineum or pelvic region, is accompanied by a violation of the normal process of urination and, in severe forms, leads to erectile dysfunction and serious problems in intercourse with a partner.
About a quarter of cases among couples suffering from infertility are precisely the causes of the male factor that affect the impossibility of conception. Male infertility is a violation of the quality of spermatozoa and their quantitative content in the ejaculate.
The prostate gland (prostate) refers to the male reproductive system. It is shaped like a chestnut, located in front of the rectum, under the bladder and surrounds the urethra (urethra). When the prostate gland becomes inflamed, it compresses the urethra, which further leads to problems with urination. The main function of the prostate is to produce a secret (fluid) that is part of the semen and dilutes it, ensuring normal sperm motility.
Prostatitis is very common in a urologist's practice. It can occur suddenly or gradually, appear constantly and for a long time (chronic prostatitis). The chronic form of this disease is more common than the acute form. Chronic prostatitis ranks fifth among the twenty leading urological diagnoses.
Since prostatitis is an active focus of infection in the body, it requires mandatory treatment, even if its symptoms do not bother you.
Reasons for the development of prostatitis
The list of causes that provoke inflammation of the prostate gland is very diverse:
- diseases of the genitourinary system (cystitis, urethritis, pyelonephritis);
- sexually transmitted infections (trichomoniasis, gonorrhea);
- infections associated with pneumonia, flu, tonsillitis, furunculosis;
- chronic constipation, forcing a man to strain regularly;
- sedentary lifestyle and irregular sex life, which lead to stagnation of the secret;
- urinary retention: a swollen bladder increases pressure on the prostate;
- frequent hypothermia (or overheating);
- injuries in the pelvic area;
- hormonal disorders that weaken the immune system.
Most often, the appearance of prostatitis is caused by pyogenic microbes: E. coli, streptococci and staphylococci, mycoplasmas, Candida fungi, Trichomonas, tubercle bacillus. They multiply very quickly and destroy prostate tissue, which is manifested by inflammation.
In most cases, the onset of prostatitis causes an infection that enters the prostate gland via the urethra. It happens that it enters the body through blood or lymph, passes from the bladder or rectum.
Important! A decrease in immunity is very dangerous for a patient with chronic prostatitis, as the prostate gland quickly becomes inflamed with fatigue, stress, lack of sleep, malnutrition and other adverse factors.
With a sedentary lifestyle and the absence of a constant sex life, the blood supply to the pelvic organs worsens, which leads to oxygen starvation of the prostate tissues and congestion. A stagnant secret is an ideal environment for the development of pathogenic microorganisms that cause inflammation.
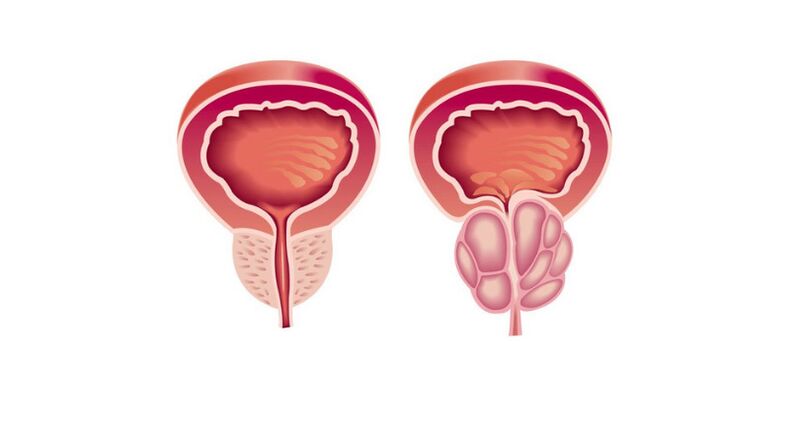
Types and forms of prostatitis
Prostatitis, depending on the cause of the disease, is classified into types and forms:
By type they are distinguished:
Bacterial prostatitis- Inflammation caused by infection. Bacterial prostatitis occurs in both young and elderly men.
congestive prostatitis- inflammation caused by stagnation of the secretion. It develops in men with a sedentary lifestyle who do not have a regular sex life. This form can be quickly supplemented by an infection and thus the stagnant process is complicated by the bacterial form.
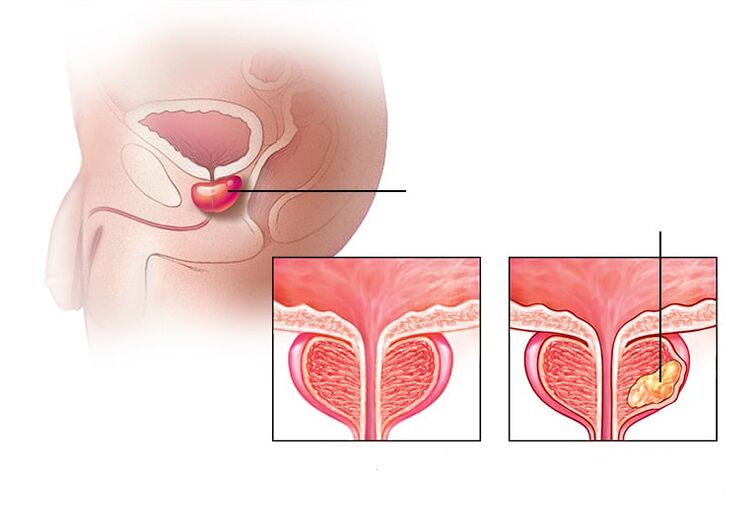
Calculous prostatitis- Stones form in the prostate gland. Untreated chronic prostatitis can cause this complication. This disease affects older men who have not followed the advice of a urologist.
According to the shape of the flow, the following are distinguished:
Acute form of prostatitis- this is an inflammation of the prostate gland caused by an infectious agent, characterized by the appearance of edema and purulent foci in the tissues. 30-58% of men of reproductive age (30-50 years) face such a diagnosis.
Chronic form of prostatitischaracterized by persistent or recurrent urogenital symptoms caused by a bacterial infection in the prostate gland. The chronic form occupies 10% of all cases of prostatitis.
Symptoms of prostatitis
Generalsymptoms of inflammation of the prostateI am:
- pain in the lumbar region;
- feelings of discomfort during intestinal motility;
- pain in the perineum or pelvic region;
- disturbances in the work of the lower urinary tract.
The acute stage of prostatitis is accompanied by a general intoxication syndrome. This disease is characterized by a strong manifestation of symptoms with a vivid clinical picture:
- a sharp rise in body temperature, chills, nausea, vomiting and malaise;
- pain syndrome and chills in the joints and muscles;
- an increase in the size of the prostate and the occurrence of discomfort in the perineal area;
- frequent urination and urinary retention.
Against the background of individual inflammatory processes, a purulent-septic disease affecting the blood can develop. In such a situation, the patient must be urgently hospitalized: with sepsis, the treatment of prostatitis should be carried out exclusively in the clinic.
Inchronic prostatitis of a bacterial naturesymptoms are usually absent, so treatment begins only when an infection in the urinary system is detected, which arises against the background of a complication of the disease. In this case, you might observe:
- pain during ejaculation;
- the appearance of blood in the ejaculate;
- the presence of discharge from the urethra;
- erectile dysfunction can develop.
If the examination did not show that chronic pain is caused by pathologies in the prostate gland, then in this case we are dealing withchronic non-bacterial prostatitisor the so-calledchronic pelvic pain syndrome. With this disease, the quality of life of a man is significantly reduced, as it leads to various ailments of a psychological and sexual nature:
- increased fatigue;
- a feeling of helplessness;
- erectile dysfunction;
- painful ejaculation;
- pain after intercourse, etc.
Similar symptoms can apply to other urological diseases, so it is impossible to diagnose prostatitis by symptoms alone. For example, urination disorders and pain are present in prostate adenoma, cystitis, various oncological tumors in the genitourinary organs, etc.
Diagnosis of inflammation of the prostate
Having identified the first signs of the inflammatory process of the prostate, the patient should immediately contact a doctor, a urologist. The doctor must exclude many diseases that have similar manifestations and determine which type of disease it belongs to.
To confirm that the patient has no other diseases (for example, appendicitis, oncology, inflammatory processes in the bladder and kidneys, prostate adenoma), the doctor must conduct the necessary examinations:
- collection of anamnesis (interrogation of the patient);
- general inspection;
- rectal examination;
- study of the secret of the prostate gland;
- tests for sexually transmitted infections;
- ultrasound examination of the prostate, scrotum and pelvic organs.
At the appointment, the urologist should clarify with the patient the duration of the clinical manifestations of the disease, the localization and nature of the pain (for example, in the perineum, scrotum, penis and inner thigh), characteristic changes in the semen (presence of pus and blood).
The doctor establishes the diagnosis of chronic bacterial prostatitis with a duration of symptoms of at least three months.
The survey will include:
- Digital rectal examination of the gland, to determine the degree of enlargement of the prostate and its consistency.
- Analysis of prostatic, urinary and / or ejaculate secretion.
- Identification of urogenital infection.
- Urodynamic study.
- Ultrasound examination of the urinary system (kidneys, prostate, bladder with determination of residual urine).
- Cultural study of prostatic secretion and microscopy of various portions of urine and prostatic secretion.
- Androflor is a comprehensive study of the microbiocenosis of the urogenital tract in men by PCR, which will determine the qualitative and quantitative composition of the microflora.
After identifying the cause of the disease, the doctor will recommend a course of treatment. It should be remembered that standard methods only in 5-10% of cases can detect an infection, which ultimately leads to prostatitis.
The patient should definitely undergo a thorough diagnosis, because the success of the treatment will depend on the accuracy of the results.
Treatment of prostatitis
When a urologist has made a diagnosis, determined the cause and form of prostatitis, she must prescribe treatment.
The main role in the treatment of this disease is assigned to drug therapy:
Antibacterial therapy
At the first stage of therapeutic therapy, it is necessary to eliminate inflammation. Antibiotics are the main treatment for acute bacterial prostatitis and are recommended for chronic bacterial prostatitis. The doctor chooses an antibacterial drug depending on which bacteria caused the disease. The patient will need to take oral antibiotics in one course for 4-6 weeks. Chronic or recurrent prostatitis takes longer to resolve. Hospitalization may be necessary for very severe manifestations, in which a course of intravenous antibiotics will be given. Usually, this happens with acute bacterial prostatitis.
Treatment with alpha1-blockers
With difficulty urinating, the doctor prescribes alpha1-blockers, which help facilitate urination and relax the muscles of the prostate and bladder. Muscle relaxants relieve pain caused by swelling of the prostate gland, which puts pressure on adjacent muscles. Non-steroidal anti-inflammatory drugs will help relieve the painful syndrome.
Also, the doctor can prescribe auxiliary drugs: biostimulants, extracts of various plants and insects in the form of rectal suppositories. Unfortunately, the use of drugs alone in the treatment of prostatitis remains insufficient.
In the treatment of this disease, the principles of the sequence of actions must be observed. Treatment of prostatitis is always complex.
Physiotherapy in the treatment of prostatitis
In the categories of chronic prostatitis, you can also use physiotherapy methods:
- massage of the prostate gland (prostate);
- laser therapy;
- hyperthermia and microwave thermotherapy;
- electrical stimulation with modulated currents with skin or rectal electrodes;
- acupuncture (acupuncture).
Alternative methods, such as hirudotherapy (treatment with medical leeches), are sometimes used to treat prostatitis, but the effectiveness and safety of this method has not been proven.
Introduction of stem cells
Cell therapy (stem cell injections) is a promising method of treating prostatitis today, it is in the early stages of development. Regarding the injection of stem cells into the prostate, we can only have hypotheses about its mechanisms and empirical data obtained from individual groups of researchers.
Surgical treatment of prostatitis
Surgical methods are used to treat complications of prostatitis (abscess and suppuration of the seminal vesicles).
Treatment of chronic pelvic pain syndrome requires separate consideration. Asymptomatic inflammatory prostatitis does not require treatment.
Diet and lifestyle for prostatitis
Prostatitis does not require a special diet, but eating a large amount of vegetables, lean meat and dairy products will help improve bowel function. It is necessary to enrich your body with a sufficient amount of fiber, foods rich in vitamin E (wheat germ, corn oil, etc. ), replace sugar with natural honey. Proper nutrition with inflammation of the prostate gland will help improve bowel function and reduce the likelihood of relapse or speed up recovery. The patient needs to limit himself to coffee, exclude alcohol, drink plenty of fluids and lead a healthy lifestyle.
Preventive measures to prevent prostatitis
When a man leads the right way of life: he follows proper nutrition, plays sports, his chances of developing chronic prostatitis are very small. The rejection of bad habits and casual sex are the prevention of this disease.
Important! There is primary and secondary prevention to prevent the development of prostatitis in men.
Primary- aimed at preventing the onset of the disease. It is about maintaining a balanced diet, a regimen of physical activity, timely treatment of any infectious diseases of the body and regular protected sexual intercourse, etc.
Secondary- aims to prevent the recurrence of existing chronic prostatitis and provides for a periodic visit by a urologist and preventive treatment with multivitamins, restoratives and sports.




























